Welcoming a Child with a Disability: What Parents Can Expect (and how to Prepare)
Parents preparing to welcome a child with a mental or physical disability are stepping into a real, holy kind of love, whether they realize it or not—one that includes grief and gratitude in the same breath. The road ahead can feel unclear, especially when medical language, school systems, and family expectations arrive all at once. This guide offers emotional, practical, and medical considerations you can expect, with concrete next steps you can take.
A steadying snapshot to hold onto
You will likely feel more than one emotion at a time: joy for your child, fear about the unknown, and a protective love that turns you into a researcher overnight. Preparation is not about controlling every outcome; it’s about building support so you can show up with steadiness. And yes—many families find that their faith deepens not because life gets easier, but because God meets them in the middle of it.
The emotional terrain nobody hands you a map for
Some parents feel immediate bonding; others feel delayed attachment because they’re in crisis mode. Both can be normal. You may also notice a cycle: hope → exhaustion → resolve → fresh questions. Give yourselves permission to process at different speeds (spouses often do). Here are common emotional waves that show up (sometimes in the same week):
● Relief after a diagnosis finally explains what you’re seeing
● Anger or sadness about losses you didn’t choose
● Guilt (“Did I cause this?”—often unfounded, but emotionally loud)
● Isolation when friends don’t know what to say
● Fierce tenderness as you learn your child’s cues and needs
If you can, ask someone you trust to pray with you in specifics: “wisdom for decisions,” “stamina for appointments,” “unity in our marriage,” “the right helpers.” Specific prayers can keep you from feeling like you’re floating.
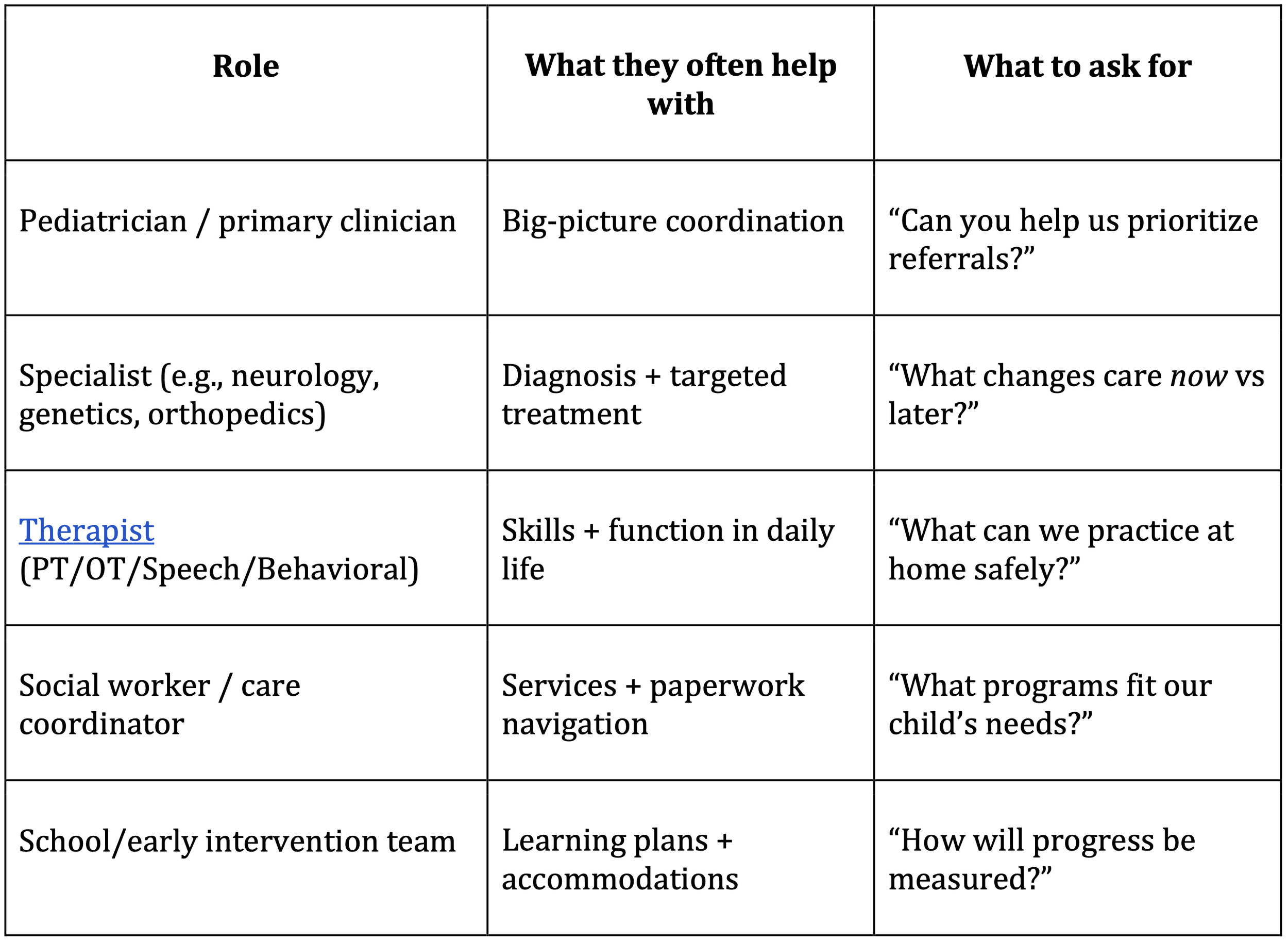
A simple “care team map”
Link to Therapists: https://www.psychologytoday.com/us/therapists
Sorting out health insurance without getting swallowed by it
Before you dive into the specifics of coverage, it helps to name the context this guidance comes from—and its limits. Much of what follows reflects North American health care systems, especially those in the United States and Canada, where insurance structures, referrals, and employer-based coverage determine how you explore your options. That said, not every country offers universal health care, consistent coverage, or predictable pathways to services. If you’re navigating systems in the UK, Europe, South Africa, or regions where health care access is fragmented or largely out-of-pocket, the details may differ, but the principles still apply. You can still look for clarity around who coordinates care, how services are accessed, what documentation matters, and where advocacy makes a difference. The goal here is not to assume one system fits all, but to offer guardrails you can adapt to the realities you’re facing—wherever you live.
How to prepare in the first 30 days
Choose one organizing system (binder, folder, app). Keep it boring and consistent.
Write a one-page summary: diagnoses (if known), meds, key symptoms, and emergency instructions.
Schedule your “anchor appointments” first (primary clinician + top-priority specialist/therapy).
Identify two support people: one for practical help (meals, rides), one for emotional/spiritual support.
Plan respite (even tiny): a weekly hour, a swap with a trusted friend, or childcare during appointments.
Talk about money plainly: expected costs, time off work, travel, and what you can pause temporarily.
FAQ
What should we tell siblings?
Offer age-appropriate truth, not a lecture. Give them a role (small, doable help) and reassurance they won’t be forgotten.
How do we handle unhelpful comments at church?
Prepare one gentle sentence you can repeat: “Thanks for caring—what we need most is prayer and practical support.” Then redirect. Are we allowed to grieve and still be grateful? Yes. Grief is not a lack of faith; it’s a human response to change and uncertainty.
What if we disagree on treatments or schooling?
Slow down and name the shared goal (“we both want our child safe and flourishing”). Consider a joint appointment with a clinician or counselor to align decisions.
One resource worth bookmarking
If you want practical support that’s also sensitive to faith, Joni and Friends offers disability ministry training and resources that can help your church become a safer place for your family—not just welcoming, but truly including. Their materials can be useful even if you’re not leading a ministry, because they put words to common barriers and offer steps to remove them.
Conclusion
You don’t have to become an expert in everything to love your child well. Build a small, reliable system: a care rhythm, a support circle, and a plan for paperwork. Expect emotional complexity—and don’t interpret it as failure. Step by step, you can prepare your home, your heart, and your community for this child you’ve been given.